Tom Forrest*
Medicinal cannabis is becoming big business in Australia despite ongoing issues for the people who need it.
“So, in the end, was it all worth it?”
“It was worth it for the kids and all the people that are alive now because I gave them the oil. And the ones that I gave a bit of extra time with their families. But the personal costs? I don’t know. I lost everything I loved. Everything. And I’m homeless now, I have literally nowhere to live. And I don’t know what I’m gonna do. But would I do it again? Yeah, I would. I would because more people’s lives were saved, you know, and that’s worth more than my life that was lost.”
Jenny Hallam was once one of Australia’s most prolific distributors of medicinal cannabis. When she discovered the apparent cure for her long-term chronic pain condition could be found in extracts of the world’s most notorious weed, she quickly set about concocting her own treatments. She became so good at it that she soon found herself crafting bespoke cannabis oils for anyone and everyone that needed her help. Her patients were people undergoing chemotherapy whose appetites returned, children with life-threatening epilepsy whose seizures vanished, and cancer patients whose tumours shrunk into nothing. Her oil was of the highest quality and she gave it all away absolutely free.
When she was caught, the judge recognised the compassionate crusade she was on but had little choice but to sentence her, if leniently. Yet, from 2015 to 2017, Hallam was essentially fulfilling the role that millions of dollars are currently being poured into trying to achieve from states and private investors alike.
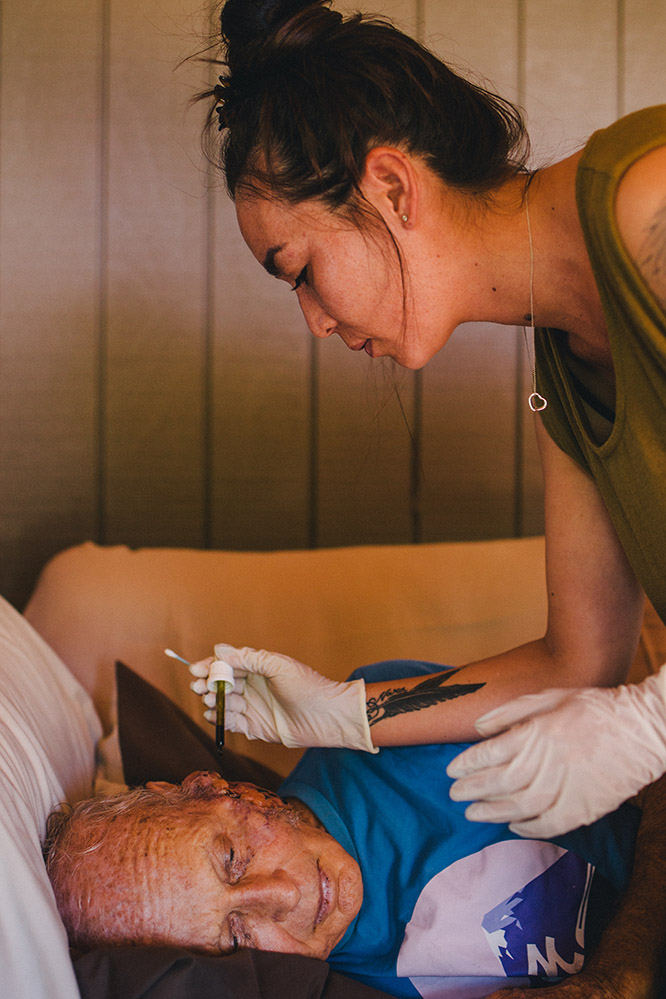
A man with a facial tumour receiving treatment. Photograph by Scott Bradshaw.
Over the past five years, the medicinal cannabis industry in Australia has undergone rapid expansion. State governments across the country are giving financial and regulatory assistance to help establish vast hectares of indoor grow operations, the result of which is thousands of tonnes of raw cannabis and millions of medically labelled bottles and packages of oils, pills, and dried cannabis flower. This is all being done as part of an explicit Federal Government strategy to make Australia one of the largest producers of medicinal cannabis on the planet – and rake in millions in tax dollars.
Patient numbers have taken off in recent years, up from just 450 in 2017 to 30,000 by the end of 2020, an increase of over 6,500%. However, while access is widening, the industry is still riddled with issues of oversight, bureaucracy, and cost. Almost all medicinal cannabis products are still classed as unapproved medicines by our federal regulatory agency, the Therapeutic Goods Administration, and as such, little is really known about what patients are receiving, how much they are paying, and what the relationships look like between suppliers and distributors.
“It’s hard to think of another sector that has such high stakes for both patients and investors and yet has such gaping holes in its implementation.”
Love Music?
Get your daily dose of everything happening in Australian/New Zealand music and globally.

It’s hard to think of another sector that has such high stakes for both patients and investors, and yet has such gaping holes in its implementation. Despite the massive increases, we are still in the early days of the wild wild west for medicinal cannabis and in the west, a lot of bad stuff went down.
Big Business
In 2016, the federal government recognised the growing body of scientific evidence and, without much warning or consultation, federally legalised the growing of cannabis for medicinal and scientific purposes. This was a validation of what the hippies have always known: cannabis is a wonder drug. From cancer to mental health, extracts and isolates of the Cannabis sativa and Cannabis indica plants have a plethora of benefits and potential cures.
Yet it’s hard not to see economics as a bigger motivating factor in the government’s decision than patient health. Very little was done in the way of getting these potentially life-saving and quality-of-life-raising medicines to those who needed or wanted them, as decisions over how to handle this new legal reality was left to the states to grapple with. Many just… didn’t.

Photograph by Tom Forrest.
With cannabis now legal, the TGA rescheduled cannabis from a Schedule 9 drug to a Schedule 8 meaning that, in theory, any doctor could apply for a prescription through the Special Access Scheme Category B pathway. The process requires specific medications to be applied for on a patient-by-patient basis, with proof that all other treatments have been exhausted, and must be signed off at the Federal and the State level.
Applying for the medication is still at the discretion of the doctor, many of whom are unfamiliar and highly sceptical of prescribing unapproved medications still tainted with associations of abuse and the dreaded but murky link to psychosis and schizophrenia. Anecdotally, patients have reported being denied medicinal cannabis for chronic pain unless they undertake a course of opiates first, for which there are good reasons to avoid.
Doctors can also become “Authorised Prescribers” by submitting a 50 page document and getting approval from an ethics committee, which the governing body of physicians in Australia doesn’t have. The title means avoiding the per-patient approval process but given the paperwork involved, few choose to do so. By 2018, there was only a single doctor licenced to prescribe medicinal cannabis in the whole country. Today there are just 148 out of roughly 40,000 GPs country-wide.
In contrast, state governments – having slowly realised the huge financial benefits to allowing and encouraging the production and sale of medicinal cannabis – are highly supportive of industrial cannabis operations. Given Australia grows some 50% of the world’s opiates, an industry worth nearly $300 million annually, the government is keen for cannabis to follow a similarly lucrative pathway.

Photograph by Tom Forrest.
Paul Mavor is a pharmacist and co-founder of Health House International, a cannabis distribution company that was granted the first medicinal cannabis import licence in Australia. He says that because “the prices have fallen out” of the opioid market, “a lot of the opium poppy growers are now looking to cannabis as the next big thing”. Australia, he argues, is “very well placed” to capitalise on the rising global demand for cannabis products “because we’ve got a clean food chain for other products like vitamins and we’re right on Asia’s doorstep. There’s a billion Chinese and a billion Indians who’ve got thousands of years of history of using cannabis as a medicine. I believe once we ramp up our industry in the right way through good manufacturing practices, there’s a very big market right there.”
“Once we ramp up our industry in the right way through good manufacturing practices, there’s a very big market right there.”
Last year, as the COVID-19 crisis was crippling our economy, the Liberal Government of Tasmania gave a $10 million commercial loan to Tasmanian Alkaloids, at the time a subsidiary of Johnson & Johnson who, in 2019, were fined almost $850 million in the US for helping to fuel the opioid crisis in the state of Oklahoma.
Michael Ferguson, the Minister for State Growth, said in a press release that the loan would deliver “new local jobs” to “recover and rebuild a stronger Tasmania” as well as “establishing our state as a recognised source of medical-grade pharmaceutical products”. Tasmanian Alkaloids are set to produce some nine million bottles of medicinal cannabis per year at its Westbury facility alone.
Tasmania is not alone in hinging at least part of its COVID-19 recovery strategy on medicinal cannabis. Queensland and Western Australia too have become hubs of medicinal cannabis production and distribution, with operations like Asterion’s $400 million venture in Toowoomba being granted Major Project Status by the Queensland Government. With the market predicted to be worth around $150 million in 2021, up from $30 million in 2019, they would be silly not to.

Photograph by Tom Forrest.
Health and politics are inextricably linked but perhaps nowhere more so than medicinal cannabis. Health minister Greg Hunt has previously stated that making Australia “the world’s number one medicinal cannabis supplier” is a key priority for the Government, and has repeatedly gone on record claiming that there are “no real government barriers at all to accessing medicinal cannabis”. Yet in 2017, when a bill was introduced in the senate to allow fast-tracked access to imported medicinal cannabis for terminally ill patients, Hunt wrote to senators urging them to deny the motion, arguing it would negatively affect the industry. The Office of Drug Control also wrote to importers in 2017 when the bill was eventually passed, stating they would be in breach of licence if they decided to supply patients though the fast-tracked scheme.
More Research Needed
“30,000 patients is not really that many, when you’ve got more than 30 companies vying for them. We used to joke that there was one patient for each company, now there’s about a thousand per company.”
Professor Ian McGregor is the head of The Lambert Initiative for Cannabinoid Therapeutics, based at the University of Sydney. When the government federally legalised the production and use of medicinal cannabis for scientific purposes, they failed to follow this up with any serious long-term research commitments. This meant the job of getting the requisite research the government required to expand patient access fell to institutions like McGregor’s – a philanthropically funded venture of the Lambert family whose granddaughter Katelyn suffers severe epilepsy.
“If you rewind to 2015 when we started this thing, everything was Schedule 9 and you needed huge amounts of paperwork and licencing,” McGregor says. “It was probably easier to deal with plutonium than with cannabis. It was nuts!”
“It was probably easier to deal with plutonium than with cannabis. It was nuts!”
“Now we seem to be in a much happier place. Medical professionals are getting more familiar with it and we’ve got about 60 ongoing clinical trials Australia-wide involving cannabinoid products. In fact, in many ways, we lead the world in clinical trials. Some of the big cannabinoid companies from America and Canada are now running their clinical trials in Australia because the regulatory environment is easier in some regards.”
While more research is an often cited claim for the delays and deferrals of the liberalisation of medicinal cannabis, McGregor argues that “although it’s true, I think you shouldn’t underestimate the amount of research that has already been done. For a lot of different conditions we can now prescribe with confidence. CBD for childhood epilepsy, that’s a no-brainer. THC/CBD for MS spasticity, there’s no argument there. Chronic pain, of course.”
“But there are huge areas that we are completely lacking in evidence and it seems so obvious that it needs to be done. Cancer is a great example. There’s not one quality clinical trial that’s been done that tells you whether cannabis extends life in people with stage four cancer. It’s just crazy if you think of the number of cancer patients that are taking cannabis around the world.”
McGregor has been at the forefront of much of the regulatory arguments and legal battles around getting greater scientific and patient access to medicinal cannabis. Rumours abound that the Lambert Initiative is not well liked by NSW Department of Health, partially due to McGregor’s forthright savaging of NSW Department of Health officials in meetings with them over their determination to drag their heels and bureaucratise progress.
The fact that it requires such outsiders and private interests to get people life-saving drugs and treatments is a recurring theme of this space. Rhys Cohen, cannabis industry consultant and editor-at-large of industry publication Cannabiz, notes that Australia is well placed to be recording tons of consumer data on how effective the cannabis medications being used are at treating the conditions they are prescribed for – none of which is being done. “We’re one of the only countries in the world that has reasonably good regulations on product quality and consistency requirements,” Cohen says. “Doctors are reporting which patient is prescribed which product for which condition, but no one in the government is collecting data on efficacy.”
Oversights like this are commonplace and leave gaps for private individuals to make up the difference. One such company is the app OnTracka, developed by social worker and cancer survivor Chad Walkaden. It benefits patients by allowing them to track their medications and set reminders to take them. This data is then anonymised and sold to companies to help them improve their products. It’s a hugely beneficial platform but one that, again, feels like it ought to come under the remit of the government rather than the private sector.

Photograph by Tom Forrest.
Other questions lie around relationships between suppliers and prescribers. Medicinal cannabis clinics – independent medical practices specialising in cannabis and the application process for getting it – are becoming big parts of the supply chain as patient numbers increase. Cohen states that most of these clinics “have a direct disclosed or undisclosed commercial relationship with a product company,” with no commercial incentive to disclose that potential conflict of interest. “It could be a violation of medical ethics,” says Cohen, “[if we knew] what actually goes on with these clinics.”
“There are several clinics that are either owned by a product company, or own their own range of products,” Cohen adds. “Whether or not doctors make decisions about which product to prescribe based on commercial incentives is unknowable because no one is auditing those decisions.”
Not only is access itself and the oversight around it a minefield, the cost of actually being treated with medicinal cannabis is still prohibitive to most. These medicines are unapproved and not covered under the Pharmaceutical Benefits Scheme, like a vast majority of what Aussies use are. This means paying market prices for a product that may not work and will require another complex application to try another.
For example, a gram of dried flower can cost anywhere from $20 to $60, something you might pay $10-15 for on the black market. Dried flower however makes up only a tiny fraction of what is often prescribed, 95% of which is oils or capsules. These more specialised medications come in at around $5-15 per day, around 20-40% higher than comparable countries with medicinal cannabis programmes.
Australia – unlike say, Canada, where companies sell directly to consumers – distributes medicinal cannabis through pharmacies. Given there are no regulations around pricing, markups for medicinal cannabis products can be as high as 30%, with the patient footing the bill for transportation and other variabilities.
Almost by definition, someone who needs medicinal cannabis to treat a chronic condition is not in a position to easily fork out $300-500 per month for treatment.
No Time to Wait
The end result of all of this red tape and medical bills is that people who need, or want, medicinal cannabis often simply resort to the black market to fill their needs. Cannabis is, after all, one of the most easily accessible illicit drugs in the country. Although advocates have been calling for it for a long time, the government still refuses to provide amnesty for medicinal cannabis users who source their medications on the black market. As a result, The Lambert Initiative recently published a study showing that only 2.7% of those using cannabis for medicinal purposes access their medication legally.
But smoking dried flower to treat chronic pain, anxiety, insomnia, or anorexia is not an exact science. You don’t know what you’re getting and you have limited ways of targeting it without getting the full-blown, and probably unwanted, side effects of the drug.
Hence why, in 2015, when Jenny Hallam began giving her unique medicines away to those in need, she had such a feeding frenzy on her hands.
“It went from, you know, a couple of people up to a couple of hundred people. As I started helping people, and it not only worked but was safe and didn’t make anybody sick, my reputation just spread. It went absolutely crazy. I was getting hundreds of requests. By the time I got raided I had a huge list of people just waiting for me to be able to supply them,” Hallam says.
“What I was doing was just trying to keep people going until the legal products were available. As soon as legal ones were available, most people didn’t need mine anymore. That was the whole idea of it. But there were people that couldn’t wait. The people that were dying of cancers, the kids with epilepsy. Any one of those seizures could be their last, any one of them could be the one that kills them. So they can’t risk just waiting for these products. To say to them ‘products will be here but it’s going to be another six months or a year’, that’s cruel. Say it to a 10-year-old kid with epilepsy and he has no chance to live. That was the problem.”

Child with epilepsy receiving CBD to treat seizures. Photograph by Scott Bradshaw
When Hallam started out, she undercut the market of those selling specialised medicinal cannabis oils which, as you might expect, ruffled a few feathers. She believes her interference in the often gang-related trade is what got her arrested.
“Another oil maker, who was charging a lot of money, wanted me out of the way because too many of their customers had stopped buying theirs and had come to me. I’ve been threatened by a lot of people including what we think are probably pharmaceutical companies. I’ve been physically attacked. I’ve had people come to my house and smash my back fence in,” Hallam says.
“I’ve been threatened by a lot of people including what we think are probably pharmaceutical companies. I’ve been physically attacked. I’ve had people come to my house and smash my back fence in.”
It’s remarkable to see the difference in willingness to put oneself in harm’s way for the sole purpose of helping other people, demonstrated by people like Hallam, when viewed in contrast to the somnambulistic approach of government. In many ways, Jenny Hallam flew too close to the sun, upset too many people, and the state made a martyr of her as a warning to other producers. But in doing so, they brought a huge amount of attention to the uses of cannabis, particularly in the over-50s, a demographic that is now the typical medicinal cannabis user.
“The black market is absolutely thriving. It’s probably tripled, at least, since my raid because there are a lot of people that didn’t realise anything about medicinal cannabis until then. That just made a whole lot of new customers. It’s definitely backfired for the government,” she says.
“The black market is absolutely thriving.”
The arbitrary and conflicted way the government has handled access to medicinal cannabis has pushed many in the community, often people with no prior knowledge or activist history, into militancy and conspiracy. Many in the broad church of medicinal cannabis users decry the influence of Big Pharma money in Australian politics, and the suppression of research and access that they see as a direct threat to the pharmaceutical industry. On the comments section of Facebook advocacy groups, it’s often hard to parse out fact from paranoia but there is likely an element of truth in some of their claims. The pharmaceutical industry stands to lose vast sums of money if medicinal cannabis is fully legalised, hence their eagerness to diversify into the burgeoning market.
One group who have managed to ride the thin line between advocacy and utility for many years without serious legal repercussions are the boys behind the 2019 documentary Green Light. Nick and Luke have both followed a similar trajectory to Hallam while, amazingly, given their brazenness in allowing their operations to be filmed, steering clear of the fuzz.
“We’ve been blessed by a huge amount of tacit support from areas of government that would otherwise be fairly punitive,” Luke says. “We’ve been tolerated because what we’re doing is the right thing for the community. I think that’s been recognised in our interactions with the government. No one has ever said, ‘You’re bad people, you’re doing the wrong thing’. What people have said is that what you’re doing is not legitimate and there are potentially serious legal outcomes should you be prosecuted. I think I would call that tolerance.”

Luke and Nick preparing to treat a patient. Photograph by Scott Bradshaw.
Their operations began over six years ago, in a similar fashion to Hallam’s, by first being switched onto the products themselves and then seeking to serve the vast numbers of “really desperate” people out there. In that time they claim to have serviced tens of thousands of people, which, if true, would be comparable to the numbers currently served by the entire Australian industry.
They specialise in “proper organic, whole plant, full-spectrum medicines” that are “grown in soil, grown in the sun, grown with rain and wind,” Nick says. Although full-spectrum medications are available legally – that’s products made using the whole plant and all its constituent cannabinoids, terpenes, and flavonoids to produce a supposedly much more beneficial “entourage effect” – many are simply isolates. That’s either THC or CBD or a mix of both by themselves, which patients, Nick tells me, “absolutely” notice the difference between. Outdoor grow operations are not currently allowed in Australia, though a few trials are underway, so much of what is accessed comes from indoor, hydroponic crops.
While Luke says he would love to go legit at some point, the barriers for doing so would require him to cease operations for up to two years while they establish themselves – not something they are likely to do anytime soon. “To desert my post as a community provider of this medicine and maybe be rewarded financially at some time in the future would be the most hollow thing that I could do with this very rich experience,” Luke says.
That’s in spite of several approaches from “very, very well resourced organisations” to “put together an IPO and an ASX listing and then float a company”. Offers, Luke claims, in the region of $20 million. That’s because, for them, the money is secondary and patient care always comes first. “If you look at it in legal terms,” Luke says, “there’s no fucking way that any remotely sane person would ever continue doing something like this unless it was deeply rewarding and enriching in so many ways more than money.”

Nick discussing treatment options with a patient. Photograph by Scott Bradshaw.
Luke doesn’t have the same fire and animosity for government and regulators that so many in this space do. On the contrary, he argues “we should have a lot of compassion for the regulators and law enforcement”. Although they are in no way “blameless”, he argues.
“We need to recognise that you’ve got people responsible for changing laws that have been so deeply entrenched in our law-and-order society for so long. For decades and decades and decades, they’ve been going out there and punitively dealing with anyone that has anything to do with these substances. To change that is a massive quantum shift.”
But, as we’ve seen, that shift is happening. Patient numbers are increasing, as is the quality and quantity of legal medicinal cannabis products, while the price and barriers to access are receding. In February 2020, the TGA created a new Schedule 3 entry for low-dose CBD, meaning medications containing up to 150mg of CBD can now be sold over the counter at pharmacies across the country. Although we will still have to wait around two years for those products to receive TGA certification, the machinery of the state does appear to be slowly creaking toward science and compassion. Yet while medicinal use of cannabis still has no amnesty, while medicines are still shielded behind layers of bureaucracy, and while patients still do not have their prescriptions subsidised under the PBS, that machinery still has a very long way to go. For many, it simply cannot move fast enough.
“Cannabis has just been so swept up in the war on drugs.”
“Cannabis has just been so swept up in the war on drugs,” Luke reminds us. “This particular war has been going on for so long and the patients are just the casualties.” Distributing medicinal cannabis has been his means of correcting this decades long “war on peace”.
“Maybe we can all grow up, we can all mature a little bit and start to see this as a human health issue in a wider sense. It’s so very evident that this is a health issue for medicinal cannabis patients. That would be a really good place to start.”